The nursing process, a cornerstone of patient care, benefits greatly from accessible PDF resources, ensuring consistent and quality documentation as initiated in BOUNTIFUL, UTAH.
What is the Nursing Process?
The nursing process is a systematic, problem-solving approach that forms the foundation of professional nursing practice. It’s a cyclical process, meaning it’s dynamic and continuously refined as a patient’s condition evolves. At its core, it involves five distinct phases: assessment, diagnosis, planning, implementation, and evaluation.
Crucially, the process begins with a thorough assessment to gather comprehensive patient data. This data then informs the nursing diagnosis, which identifies specific patient responses to actual or potential health problems. Following diagnosis, a care plan is developed with measurable goals and targeted interventions.
Implementation involves carrying out those interventions, and finally, evaluation determines the effectiveness of the plan, leading to adjustments as needed. Utilizing a Nursing Process PDF streamlines documentation, ensuring all phases are consistently addressed, as highlighted in resources originating from locations like BOUNTIFUL, UTAH.
Importance of a Nursing Process PDF Resource
A dedicated Nursing Process PDF resource is invaluable for several reasons. It standardizes documentation, ensuring all essential elements of patient care are consistently recorded, a practice particularly emphasized in settings like BOUNTIFUL, UTAH. PDFs facilitate easy sharing and archiving of care plans, promoting seamless communication among healthcare team members.
Furthermore, PDF templates can be pre-populated with common nursing diagnoses and interventions, saving valuable time and reducing the risk of errors. Digital forms within PDFs allow for efficient data entry and organization, improving overall workflow.
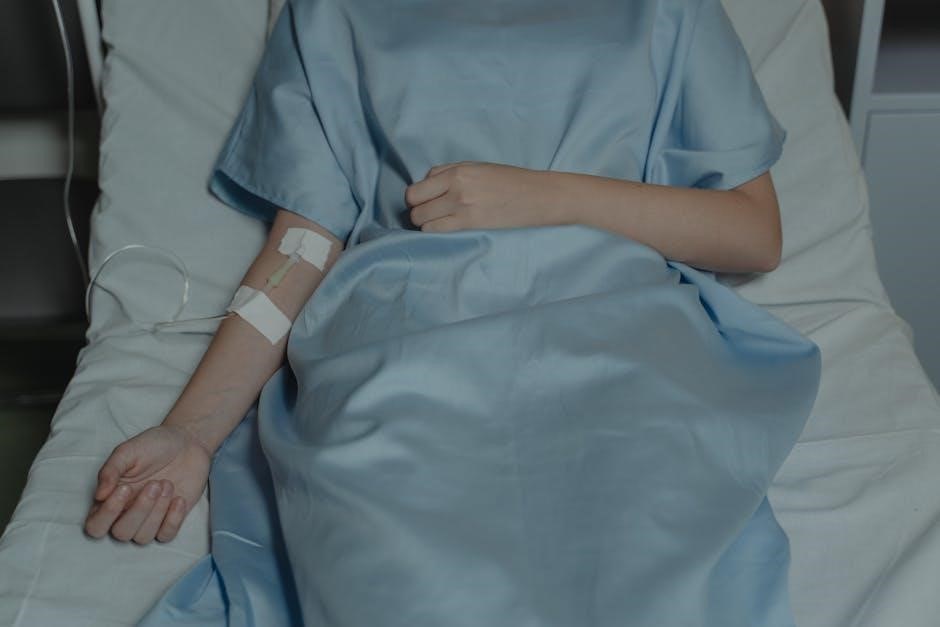
The accessibility of PDFs across various devices ensures that care plans are readily available at the point of care, supporting informed decision-making and enhancing patient safety. Ultimately, a well-designed Nursing Process PDF contributes to higher quality, more coordinated, and legally sound patient care.

Phase 1: Assessment
The initial assessment phase, crucial for care planning, is streamlined with Nursing Process PDFs, enabling thorough data collection and analysis for optimal outcomes.
Data Collection Methods
Effective data collection is the bedrock of the assessment phase, and utilizing Nursing Process PDFs can significantly enhance this process. Several methods are employed, including patient interviews – a primary source for subjective data – and physical examinations yielding objective findings.
Observation skills are paramount, noting non-verbal cues and environmental factors. Reviewing existing medical records, including previous assessments and diagnostic results, provides valuable context. PDFs serve as excellent templates for standardizing data collection, ensuring all relevant information is consistently captured.
Furthermore, incorporating family member input, when appropriate, offers a holistic view of the patient’s condition. Utilizing structured PDF forms can guide data gathering, minimizing omissions and promoting comprehensive assessments. These PDFs can be easily integrated into Electronic Health Records (EHRs) for seamless documentation.
Subjective vs. Objective Data
Distinguishing between subjective and objective data is fundamental to accurate assessment, and Nursing Process PDFs can aid in organized recording. Subjective data encompasses what the patient tells you – their feelings, perceptions, and descriptions of symptoms. This is inherently personal and cannot be independently verified.
Conversely, objective data consists of measurable and observable facts – vital signs, lab results, physical examination findings. These are independent of the patient’s perception.
PDF documentation forms should clearly delineate sections for both data types. Utilizing standardized PDF templates ensures consistent collection and prevents mixing of subjective and objective information. Accurate differentiation is crucial for formulating appropriate nursing diagnoses and developing effective care plans. A well-structured PDF facilitates this critical analysis.
Utilizing PDF Forms for Data Gathering
PDF forms offer a standardized and efficient method for collecting patient data during the assessment phase of the nursing process. Pre-designed PDF templates can include fields for vital signs, medical history, allergies, and current medications, streamlining the data gathering process.
These forms promote consistency across different nurses and settings, reducing errors and omissions. Fillable PDF forms allow for direct input, minimizing handwriting legibility issues.
Furthermore, PDFs can be easily integrated into Electronic Health Records (EHRs), facilitating seamless data transfer and storage. Customizable PDF templates can be tailored to specific patient populations or clinical settings, enhancing their utility; Properly designed PDFs improve data quality and support informed decision-making.
Electronic Health Records (EHR) Integration & PDFs
Seamless integration between Electronic Health Records (EHRs) and PDF documents is crucial for modern nursing practice. PDFs serve as a versatile medium for sharing information from and to EHR systems, ensuring data accessibility and continuity of care.
Nurses can export patient data from EHRs into PDF reports for easy sharing with other healthcare professionals or for documentation purposes. Conversely, completed PDF forms – like assessment data – can be imported directly into the EHR, reducing manual data entry.
This integration minimizes redundancy, improves accuracy, and enhances workflow efficiency. Secure PDF formats protect patient confidentiality while facilitating information exchange. Utilizing PDFs within an EHR ecosystem supports a comprehensive and well-documented nursing process.

Phase 2: Diagnosis
Accurate nursing diagnoses, often utilizing NANDA-I classifications, are essential; PDF templates streamline documentation of the diagnostic process and PES statement formulation.
Defining Nursing Diagnoses (NANDA-I)
NANDA-I (North American Nursing Diagnosis Association International) provides a standardized, globally recognized vocabulary for nursing diagnoses. Utilizing this framework ensures clarity and consistency in identifying patient health problems. These diagnoses aren’t medical diagnoses; rather, they describe the nurse’s clinical judgment concerning a human response to actual or potential health problems.
PDF resources can greatly assist in applying NANDA-I. Comprehensive lists of approved diagnoses, with defining characteristics and related factors, are readily available in PDF format. These PDFs allow nurses to quickly reference and select the most appropriate diagnosis based on patient assessment data. Furthermore, utilizing standardized terminology improves communication among healthcare professionals and facilitates accurate documentation within Electronic Health Records (EHRs).
PDFs offer a convenient way to access and implement NANDA-I, promoting best practices and enhancing the quality of patient care. They are invaluable tools for both experienced nurses and students learning the diagnostic process.
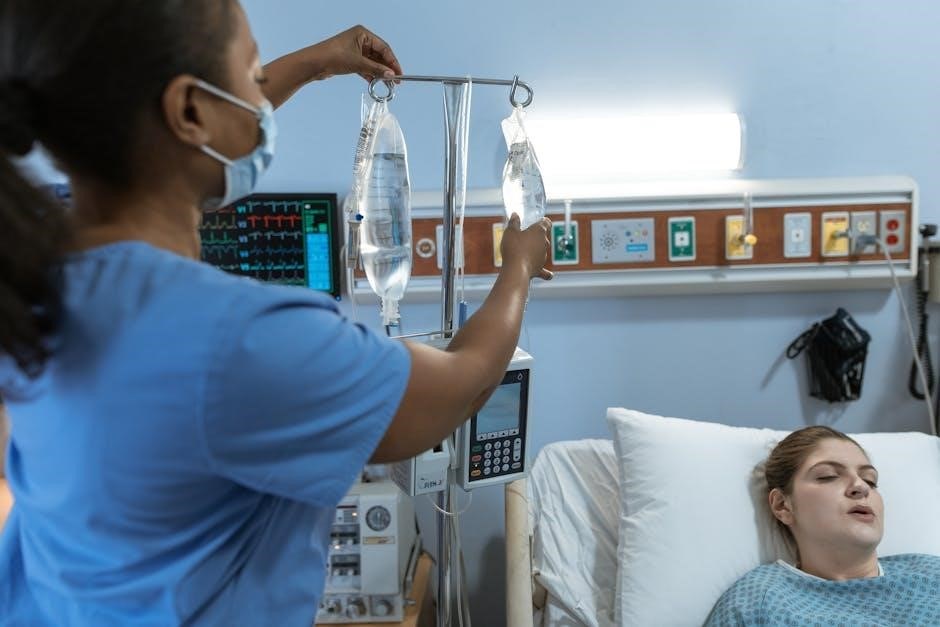
Formulating a PES Statement
A PES statement is the foundation of a nursing diagnosis, providing a concise and standardized description of the patient’s health problem. PES stands for Problem, Etiology, and Signs/Symptoms. The ‘Problem’ identifies the nursing diagnosis, the ‘Etiology’ describes the cause or contributing factors, and ‘Signs/Symptoms’ are the evidence supporting the diagnosis.
PDF templates can streamline PES statement creation. These templates provide a structured format, prompting nurses to clearly articulate each component. Utilizing a PDF ensures all necessary elements are included, promoting thoroughness and accuracy. A well-formulated PES statement guides intervention planning and facilitates effective communication.
PDFs offer a practical tool for documenting PES statements within the nursing process. They support consistent application of the NANDA-I framework and contribute to comprehensive patient care documentation, improving overall quality.
PDF Templates for Nursing Diagnosis Documentation
Utilizing pre-designed PDF templates significantly enhances the efficiency and standardization of nursing diagnosis documentation. These templates provide a structured format, ensuring all critical elements – the PES statement, related factors, and defining characteristics – are consistently recorded.
PDF templates minimize errors and omissions, promoting clarity and accuracy in patient records. They can be customized to align with specific institutional policies and NANDA-I guidelines. Furthermore, PDFs facilitate easy sharing and integration with Electronic Health Records (EHRs).
Accessible templates streamline workflow, allowing nurses to focus on patient care rather than struggling with documentation format. PDFs offer a secure and reliable method for maintaining a comprehensive and organized record of nursing diagnoses throughout the care continuum.
Prioritizing Nursing Diagnoses
Effective patient care hinges on the ability to prioritize nursing diagnoses, addressing the most urgent and life-threatening concerns first. This process demands critical thinking and a thorough understanding of the patient’s condition.
Utilizing a framework like Maslow’s Hierarchy of Needs can guide prioritization, focusing on physiological needs before safety, love/belonging, esteem, and self-actualization. PDF documentation tools can incorporate prioritization fields, prompting nurses to rank diagnoses based on severity and immediacy.
Clear documentation within the PDF, outlining the rationale for prioritization, is crucial for continuity of care and effective communication among the healthcare team. Prioritization ensures resources are allocated efficiently, maximizing positive patient outcomes.

Phase 3: Planning
Strategic planning, facilitated by PDF checklists and individualized care plans, establishes SMART goals and targeted nursing interventions for optimal patient well-being.
Setting SMART Goals
Establishing SMART goals – Specific, Measurable, Achievable, Relevant, and Time-bound – is paramount within the planning phase of the nursing process. Utilizing PDF templates can streamline this process, providing a structured format to clearly define desired patient outcomes.
A Specific goal pinpoints exactly what needs to be accomplished. Measurable aspects allow for objective tracking of progress, often documented within the PDF care plan. Achievable goals are realistic for the patient’s capabilities and resources. Relevant goals align with the overall nursing diagnosis and patient needs, ensuring focused care.
Finally, Time-bound goals establish a clear timeframe for achievement. PDF documentation facilitates consistent monitoring and evaluation against these pre-defined SMART criteria, enhancing the effectiveness of the nursing intervention and overall patient care quality.
Developing Nursing Interventions
Crafting effective nursing interventions is central to the planning phase, and PDF resources offer a structured approach to detail these actions. Interventions should directly address the identified nursing diagnoses, aiming to achieve the established SMART goals.
PDF checklists can be invaluable, prompting nurses to consider a comprehensive range of interventions – pharmacological, non-pharmacological, educational, and supportive. These checklists ensure no crucial step is overlooked.
Detailed documentation within the PDF care plan is essential, outlining what interventions will be performed, how they will be implemented, when they will occur, and who is responsible. This clarity promotes consistency and accountability, ultimately improving patient outcomes and care coordination.
PDF Checklists for Intervention Planning
Utilizing PDF checklists streamlines the development of nursing interventions, ensuring a systematic and thorough approach to care planning. These checklists serve as valuable prompts, guiding nurses to consider all relevant aspects of intervention selection and implementation.
A well-designed PDF checklist might include categories like medication administration, wound care, patient education, mobility assistance, and psychological support. Each category would list specific actions to consider, tailored to the patient’s diagnosis and needs.
PDF format allows for easy customization and integration into existing care plans. Checklists promote consistency among nursing staff, reduce the risk of errors, and facilitate comprehensive documentation, ultimately enhancing the quality and safety of patient care.
Individualized Care Plans in PDF Format
Creating individualized care plans in PDF format offers a centralized and easily shareable document for comprehensive patient management. This digital approach facilitates seamless communication among healthcare team members, ensuring everyone is aligned on the patient’s goals and interventions.
PDF care plans can incorporate various elements, including nursing diagnoses, SMART goals, planned interventions, medication schedules, and evaluation criteria. The format allows for the inclusion of electronic signatures for verification and accountability.
Furthermore, PDF’s portability enables access to care plans at the point of care, improving efficiency and reducing the potential for errors. Consistent use of PDF care plans promotes standardized, high-quality care delivery.

Phase 4: Implementation
Implementation involves actively performing the planned interventions, meticulously documented in PDF reports, ensuring patient safety and effective care delivery throughout the process.
Performing Nursing Interventions
Successfully executing nursing interventions requires skill, precision, and a deep understanding of the patient’s condition. This phase translates the carefully planned interventions into direct patient care actions. Interventions can range from administering medications and providing wound care to offering emotional support and educating patients and their families.
Effective performance necessitates adherence to established protocols and best practices, while remaining flexible to adapt to the patient’s evolving needs. Clear communication with the healthcare team is paramount, ensuring everyone is informed about the interventions being performed and any observed changes in the patient’s status.
Detailed documentation within PDF reports is crucial, recording not only what interventions were performed, but also how they were carried out, the patient’s response, and any unexpected outcomes. This comprehensive record serves as a legal document and facilitates continuity of care.
Documentation of Interventions in PDF Reports
Meticulous documentation of nursing interventions within PDF reports is a non-negotiable aspect of professional practice. These reports serve as a legal record, demonstrating the care provided and its impact on the patient’s well-being. PDFs offer a standardized, secure, and easily shareable format for this critical information.
Entries should be factual, objective, and comprehensive, detailing what intervention was performed, the time it was administered, the route (if applicable), the dosage, and, crucially, the patient’s response. Any adverse reactions or unexpected outcomes must be documented immediately and thoroughly.
Utilizing pre-formatted PDF templates streamlines this process, ensuring all necessary elements are included. Accurate and timely documentation supports effective communication, facilitates continuity of care, and protects both the patient and the nurse.
Delegation and Supervision
Effective delegation is a vital skill within the nursing process, and proper documentation within PDF reports is paramount. Nurses retain accountability for delegated tasks, necessitating clear communication and thorough supervision. Utilizing PDF checklists can aid in verifying competency of the delegated personnel before assignment.
When delegating, the nurse must assess the delegatee’s skill level and knowledge base, ensuring they are capable of safely performing the task. The delegation process, including the specific task, expected outcomes, and reporting requirements, should be clearly documented in the patient’s PDF care plan.
Regular supervision and follow-up are essential, with any observations or concerns promptly recorded within the PDF. This ensures patient safety and demonstrates responsible nursing practice.
Maintaining Patient Safety During Implementation
Patient safety is the highest priority during the implementation phase of the nursing process, and comprehensive PDF documentation plays a crucial role. Accurate recording of interventions, including medication administration, wound care, and patient education, within PDF reports is essential for tracking and preventing adverse events.
Utilizing standardized PDF forms can minimize errors and ensure all necessary information is captured. Double-checking medications, verifying patient identification, and adhering to infection control protocols are vital, with any deviations or incidents immediately documented in the patient’s PDF record.
PDF-based incident reporting systems facilitate prompt investigation and corrective action, contributing to a culture of safety and continuous improvement.

Phase 5: Evaluation
The final phase utilizes PDF tools for reporting goal achievement and analyzing data, enabling nurses to revise care plans for continuous quality improvement.
Evaluating Goal Achievement
Evaluating goal achievement is a critical step within the nursing process, determining the effectiveness of implemented interventions. Utilizing a Nursing Process PDF allows for structured documentation of patient responses and progress towards established outcomes. This involves objectively measuring if the patient has met the SMART goals defined during the planning phase.
PDF forms can be designed with specific criteria for evaluation, prompting nurses to document observable changes in patient condition. These forms facilitate a consistent and thorough assessment, reducing subjectivity and ensuring accountability. The evaluation should consider not only whether the goal was met, but also the degree to which it was achieved and any barriers encountered.
PDF reports generated during evaluation provide a clear record of the patient’s journey and inform future care decisions. This data is invaluable for continuous quality improvement initiatives and demonstrates the value of a well-documented nursing process.
Analyzing Data & Revising the Care Plan
Following evaluation, a thorough analysis of collected data is essential to determine the effectiveness of the nursing care plan. A Nursing Process PDF streamlines this process, providing a centralized location for all relevant patient information and evaluation findings. If goals were not fully met, or new problems arise, the care plan requires revision.
PDF templates can incorporate sections for documenting the rationale behind revisions, ensuring transparency and promoting collaborative care. This analysis should identify factors contributing to both successes and failures, informing adjustments to interventions and goals.
Utilizing PDF tools allows for easy modification and version control of the care plan, maintaining a clear audit trail. Revising the plan isn’t a failure, but a demonstration of responsive, patient-centered care, continually optimized through data-driven insights documented within the PDF.
PDF Tools for Evaluation Reporting
Efficient evaluation reporting hinges on accessible and user-friendly tools, and Nursing Process PDFs excel in this area. Specialized PDF software allows for the creation of standardized evaluation forms, ensuring consistent data collection across patients. These forms can include pre-populated fields, drop-down menus, and scoring systems, simplifying the documentation process.
PDF editors facilitate the addition of charts, graphs, and narrative summaries to visually represent evaluation findings. Features like commenting and highlighting enable collaborative review and feedback from the care team.
Furthermore, PDFs support secure sharing and archiving of evaluation reports, maintaining confidentiality and facilitating quality improvement initiatives; Utilizing these tools transforms evaluation from a cumbersome task into a streamlined, data-driven process, enhancing patient outcomes.
Continuous Quality Improvement & the Nursing Process
The Nursing Process, when documented effectively using PDFs, becomes a powerful engine for Continuous Quality Improvement (CQI). Standardized PDF forms facilitate data collection across patient cases, enabling identification of trends and areas for enhancement. Analyzing aggregated data from these PDFs reveals patterns in care delivery and patient outcomes.
PDFs allow for easy tracking of interventions and their effectiveness, supporting evidence-based practice. Regular review of PDF-documented care plans and evaluations identifies gaps in care and opportunities for protocol refinement.
This data-driven approach fosters a culture of learning and improvement, ultimately leading to higher quality patient care and optimized resource utilization. The structured nature of PDF documentation streamlines CQI efforts, making them more efficient and impactful.

PDF Resources & Tools
Numerous free and commercial PDF templates and software solutions streamline the nursing process, enhancing documentation and care plan accessibility for nurses.
Free Nursing Process PDF Templates
Accessing free Nursing Process PDF templates offers a cost-effective starting point for many healthcare professionals. These readily available resources often include basic assessment forms, nursing diagnosis lists aligned with NANDA-I, and simple care plan outlines.
Several websites and nursing education platforms provide downloadable templates covering various specialties, such as medical-surgical, pediatric, and mental health nursing. While these templates may lack the advanced features of paid software, they are invaluable for students, new graduates, or facilities with limited budgets.
However, it’s crucial to verify the template’s accuracy and alignment with current best practices. Always supplement free templates with institutional policies and individual patient needs, ensuring comprehensive and individualized care documentation.
Commercial Nursing Process PDF Software
Investing in commercial Nursing Process PDF software provides robust features for streamlined documentation and enhanced care coordination. These platforms typically offer customizable templates, integrated drug databases, and automated charting capabilities, significantly reducing administrative burden.
Many software solutions facilitate Electronic Health Record (EHR) integration, allowing seamless data transfer and minimizing redundant documentation. Advanced features include automated nursing diagnosis suggestions based on assessment data, collaborative care planning tools, and comprehensive reporting functionalities.
While requiring a financial investment, commercial software often delivers a substantial return through improved efficiency, reduced errors, and enhanced compliance. Consider factors like scalability, user-friendliness, and vendor support when selecting a suitable solution for your healthcare setting.
Legal Considerations for PDF Documentation

Maintaining meticulous and legally sound PDF documentation is paramount in nursing practice. Healthcare professionals must adhere to HIPAA regulations regarding patient privacy and data security when creating, storing, and transmitting PDF records.
Proper authentication and audit trails are crucial; ensure PDF software supports digital signatures and tracks all document modifications. Accurate and objective documentation, free from alterations or subjective interpretations, is essential for legal defensibility.
Retention policies must comply with state and federal guidelines, specifying the duration for which PDF records must be preserved. Understanding legal precedents related to nursing documentation and utilizing standardized templates can mitigate risk. Regular staff training on proper PDF documentation practices is vital for maintaining compliance.